Helping your pets live their best lives
Helping your pets live their best lives
Providing your pets with
a better lifestyle, together
CONTACT US 045 521507 its@apetslife.ie

GYM DOG
Gym Dog is Ireland’s first pet resort where you will find an onsite hospital, boarding kennels, daycare centre, dog park, dog gym and wellness centre. Gym Dog is home to veterinary professionals serving clients in the surrounding areas.
KILDARE VET SURGERY
WE CARE
Kildare Vet Surgery is a family owned veterinary practice located in Kildare. We have a dedicated team of veterinary professionals serving clients in the surrounding areas.
GymDog and GymCat all natural diets developed
by Dr Des Groome
Champions
of pet welfare
We are proud to boast that we are Ireland’s first ever pet resort. We monitor every aspect of your pets health, exercise routine, eating habits and behaviour. This means all aspects of their care are catered for under our guidance and supervision.



Sometimes the best medicine is the unconditional love from your pet
Your pets happiness and lifelong health depends on how well their natural needs and instincts are being fulfilled.
Our Happy Customers


"Bertie has been a regular at Gym Dog for nearly 1.5 years. He adores it there. When we first adopted him, he was hyper and was hard to deal with in our home. Thankfully, Gym Dog saved our sanity and gave Bertie that mental and physical exertion that he needs. We now have a (mostly) calm dog in our home. Thank you to all the wonderful staff there."
– Elaine

"We started taking Lola to Gym Dog in 2021, Lola loves to run and at a fast speed. We met Des and explained we wanted her to run freely and come home tired which she does every time! All the Gym Dog girls are amazing and so caring towards Lola. Lola can’t wait to get out the car when we arrive (sometimes even through the car window!) and nearly wags herself in half every time she sees the girls. We couldn’t recommend Gym Dog daycare and boarding enough, a proper doggy paradise!"
– Craig

"My Alsatian Black German Shepard, Pablo, enjoys every single moment spent at Gym Dog , he made friends and always give kisses to the girls who are looking after them . This means a lot! And the most important thing is that he’s tired when is at home and we can all have a peaceful night sleep!"
– Elena
Vets and Their Pets
2024 PRICES
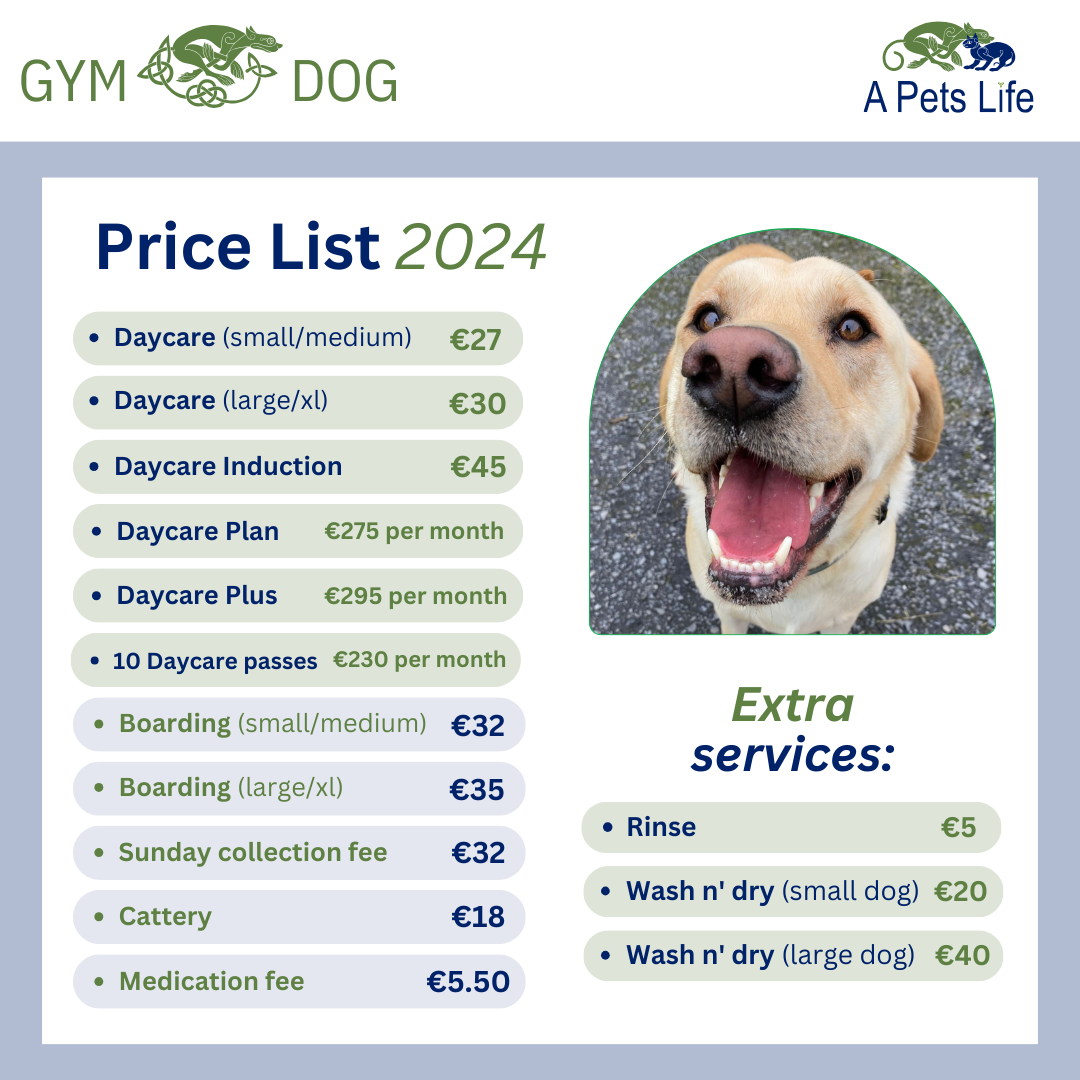
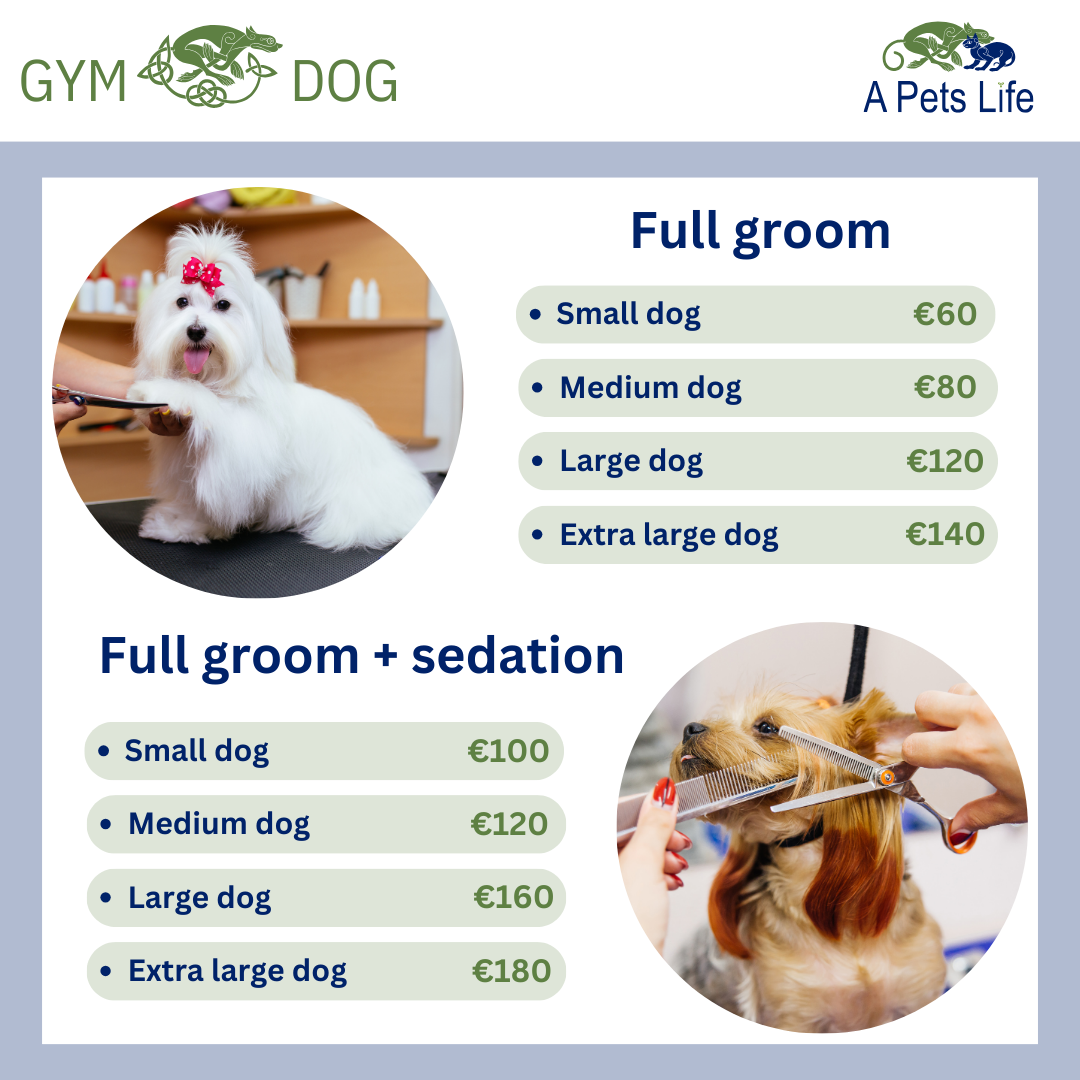


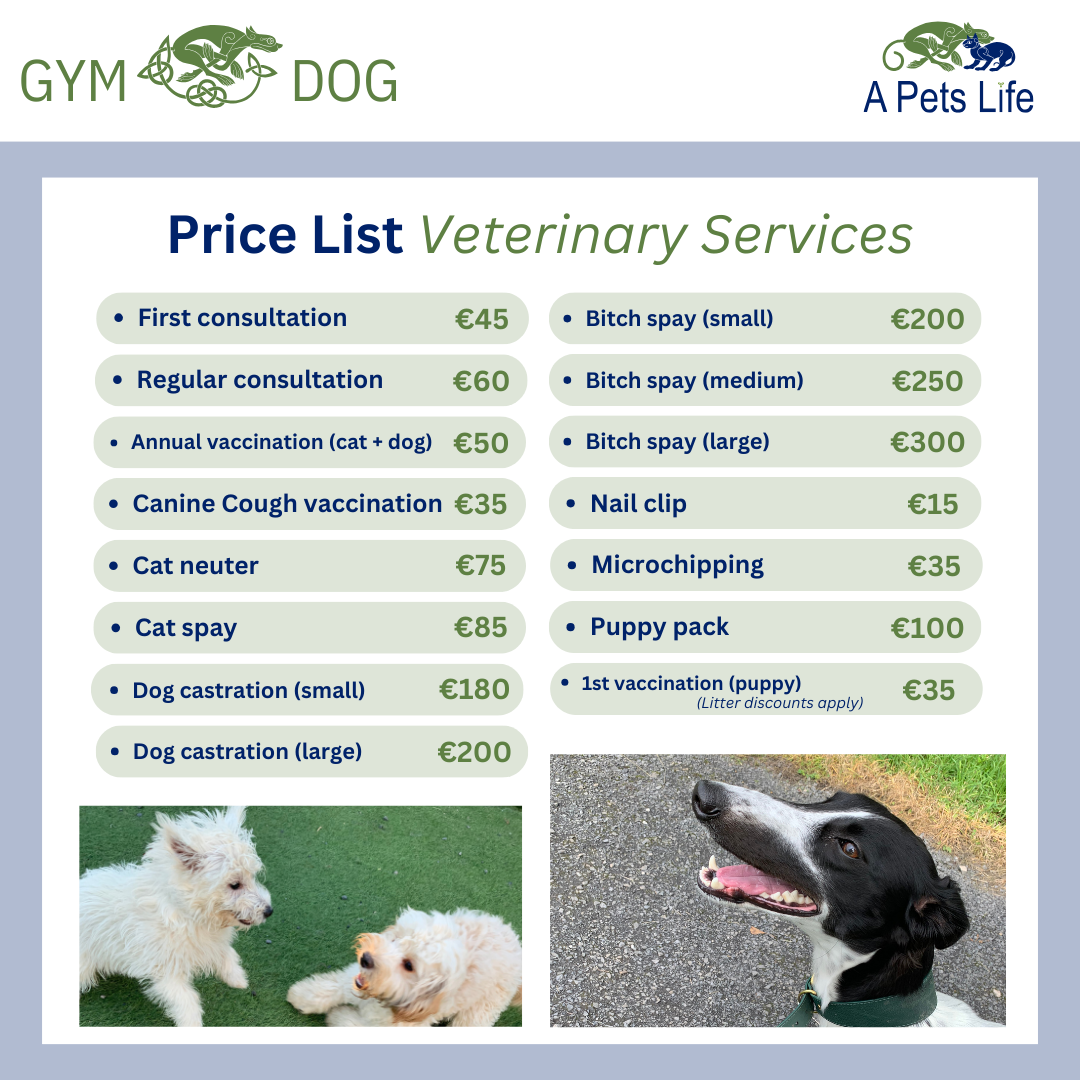


NEW Premium Health Plans 2024


















